
For those geriatric and palliative care practitioners who glossed over the recent NEJM publication of the Heartmate II trialas yet another esoteric, hyper-specialized trial should think twice. This trial could have significant implications for many geriatric and palliative care patients.
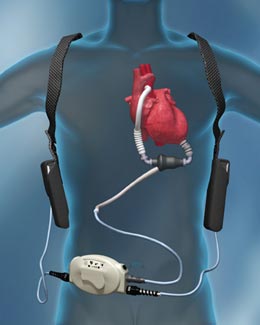
Issue #1 – disconnecting the Left Ventricular Assist Device (LVAD): On our palliative care service, I recently assisted with the care of a 74 year-old gentleman with one of these continuous flow LVADs. It was one of the most complicated goals-of-care discussions I have ever been involved with. From a cardiac standpoint, his heart/LVAD were doing extremely well. He did not have any signs of infection and his LVAD was maintaining great cardiac output. That said, He kept getting admitted with mild flare-ups of acute pancreatitis of unknown etiology, he didn’t want to get out of bed, and had an albumin of 2.8. Ultimately, he refused SNF, went home, failed rehab at home, stopped performing his ADLs, and transitioned to hospice. He then began requesting that they disconnect the LVAD. Because he wasn’t having any “problems” with his LVAD, there was reluctance to disconnect despite his near complete lack of function. Ultimately, the device nurse went to visit him at home and agreed that “he was done” and disconnected the LVAD. He died 5 minutes later. Earlier in the course of his illness, this same device nurse astutely noted “every destination LVAD will eventually require an end-of-life discussion.”
Issue # 2 – determining who would benefit from the LVAD: In the aftermath of this case, the cardiologists here in Colorado raised the question of whether they could predict, based on pre-procedure functioning, those who are too frail to benefit from an LVAD (yes, the cardiologists here in Colorado are far ahead of their field in considering geriatric and palliative care issues). In thinking about this further, I have realized a significant challenge. Defining a population unlikely to benefit from LVAD because of frailty (which makes perfect sense in decisions like colon or breast cancer screening) will be more difficult here as the frail will also be the population that stands to benefit the most. Indeed, patients in the trial improved a 6 minute walk from an average of 182 meters at baseline to 372 meters at 24 months – and these patients were sick (ineligible for transplant, failed medical management, at least 14 days of inotropes, etc.) Thus, LVADs appear to actually treat frailty…?
I write this post for a couple of reasons. First, I think the palliative care community needs to consider the unique challenges involved in disconnecting LVADs; while I think we are quite comfortable disconnecting ventilators and turning ICDs off, for some reason, LVADs feel different. Perhaps it is because this life-support is so directly tied to cardiac output. Perhaps the type of person who would accept an LVAD for destination therapy has a pre-disposition to defer end-of-life discussions. Second, some of the contributors to this blog are experts in using functional measures to predict outcomes and I would love to hear their thoughts on the use of ‘frailty’ to determine who might fail an LVAD.



